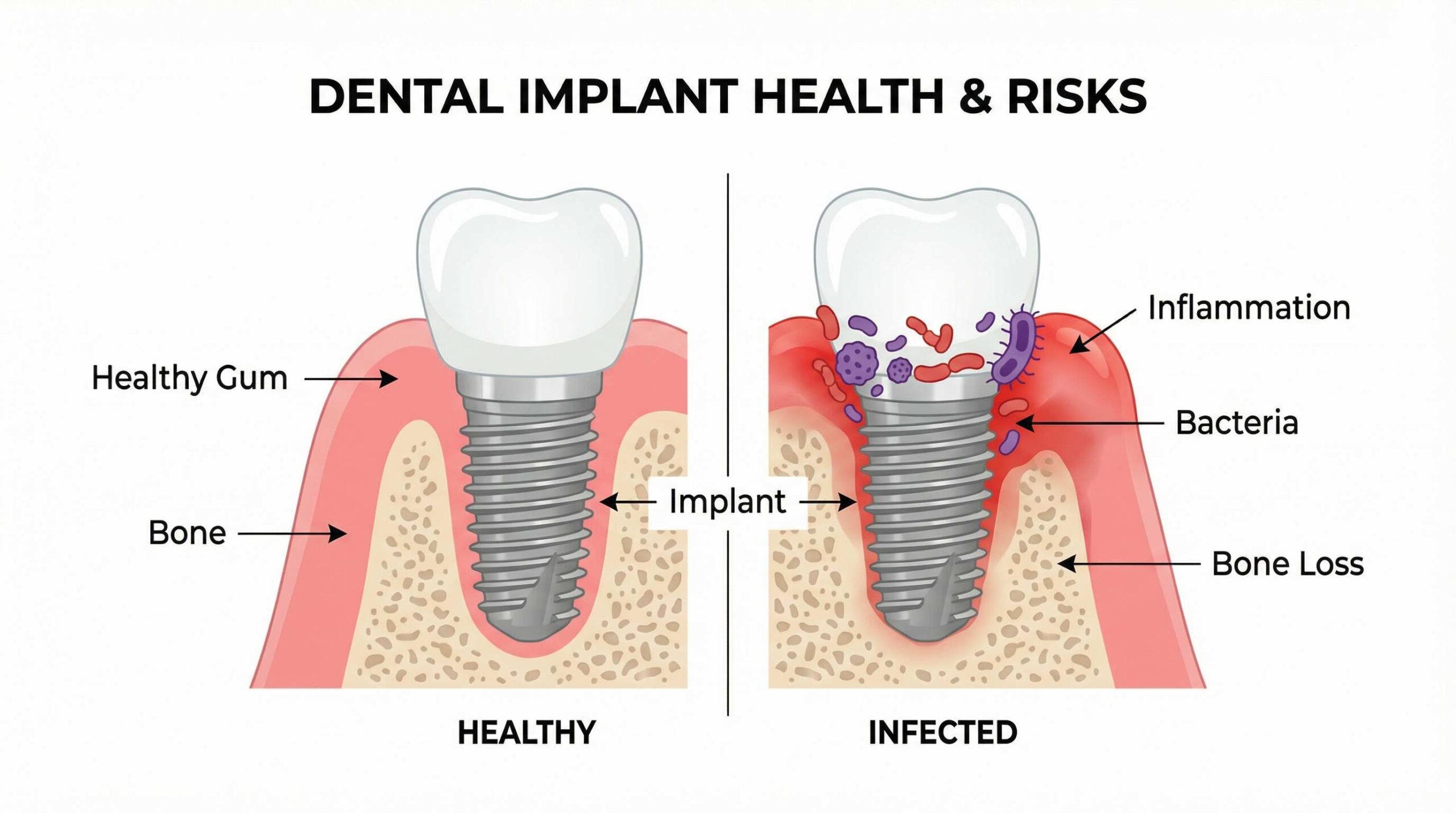
When you receive an implant—whether it’s a dental fixture to restore your smile or a medical device like a hip replacement—the goal is a better quality of life. However, your body’s interaction with these foreign objects isn’t always seamless.
One of the most significant hurdles to a successful recovery is an implant infection. Understanding the warning signs and acting early can be the difference between a simple fix and a complex secondary surgery.
What is an Implant Infection?
An implant infection occurs when harmful bacteria colonize the area around a surgically placed device. In the dental world, this is often called peri-implantitis.
Unlike natural tissue, implants lack a natural blood supply to deliver immune cells directly to the surface of the material. This makes it easier for bacteria to form a “biofilm”—a protective layer that shields them from your body’s natural defenses and even some antibiotics.
The Two Critical Windows
-
Early Infection (Post-Op): Usually occurs within weeks of surgery, often due to bacterial contamination during the procedure or poor initial healing.
-
Late Infection: Can occur months or even years later. This is often triggered by bacteria traveling through the bloodstream from another part of the body or poor long-term maintenance.
Symptoms You Should Never Ignore
Early detection is the “gold standard” for saving an implant. If you notice these symptoms, contact your specialist immediately:
-
Persistent Pain: While some discomfort is normal after surgery, pain that intensifies after the first week is a red flag.
-
Swelling and Redness: Gums or skin around the site that appear angry, bright red, or feel hot to the touch.
-
Pus or Discharge: Any yellowish or white fluid (exudate) oozing from the implant site.
-
Unpleasant Taste or Breath: A persistent metallic taste or foul odor that doesn’t go away with brushing.
-
Instability: If the implant feels like it is shifting, clicking, or “loose,” the supporting bone may be compromised.
-
Systemic Signs: Fever, chills, or swollen lymph nodes indicate the infection may be spreading.
Common Causes & Risk Factors
Why do some implants fail while others last a lifetime? Several factors can increase your vulnerability:
| Factor | Impact on Implant |
| Smoking | Constricts blood flow, significantly slowing the healing process. |
| Diabetes | Uncontrolled blood sugar can impair the body’s ability to fight off oral or surgical bacteria. |
| Poor Hygiene | Plaque buildup around dental implants is the #1 cause of peri-implantitis. |
| Autoimmune Issues | A compromised immune system may not be able to prevent bacterial colonization. |
| Parafunctional Habits | Teeth grinding (bruxism) can create micro-gaps where bacteria hide. |
Treatment: Can an Infected Implant Be Saved?
The short answer is yes, but timing is everything. Treatment typically follows a tiered approach:
1. Non-Surgical Debridement
For early-stage infections, a professional deep cleaning using specialized tools (that won’t scratch the implant surface) can remove the bacterial biofilm. This is often paired with local or systemic antibiotics.
2. Laser Therapy
Advanced clinics often use lasers to decontaminate the surface of the implant. The laser energy kills bacteria in hard-to-reach microscopic “pores” of the implant material without damaging the surrounding tissue.
3. Surgical Intervention
If bone loss has occurred, a surgeon may need to open the area to clean the implant directly. In some cases, a bone graft is performed to rebuild the lost support structure.
4. Removal (The Last Resort)
If the implant has lost significant bone integration and is “spinning” or loose, it may need to be removed. Once the area heals and the infection is cleared, a new implant can often be placed.
Prevention: Protecting Your Investment
Preventing an infection is far easier (and cheaper) than treating one.
-
Use a Water Flosser: Especially for dental implants, water flossers can reach “pockets” that traditional floss might miss.
-
Cessation of Smoking: If you are getting an implant, quitting smoking is the single best thing you can do for its longevity.
-
Regular Monitoring: See your specialist at least twice a year. They use X-rays to check bone levels that you can’t see in the mirror.